
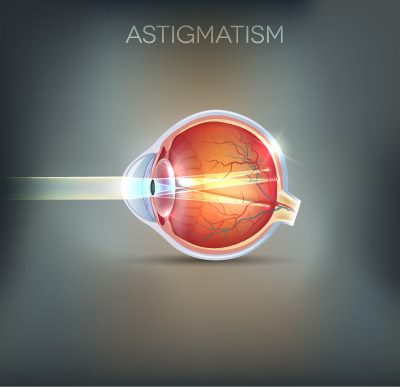
Astigmatism
Astigmatism is a condition where the eyeball is an unusual shape. Astigmatism can cause blur at all distances, and some directions in an image are more out of focus than others. This can be contrasted with short-sightedness (myopia) where all directions are uniformly blurred.
Most astigmatism is caused by the shape of the front surface of the eye (the cornea). It can also be caused by slight tilting of the lens inside the eye. It may be an inherited characteristic or a normal variation accompanying growth.
Spectacles and contact lenses (hard and soft) can correct astigmatism. It may take a week or so to adjust to astigmatic correction.
Most people have a slight amount of astigmatism.
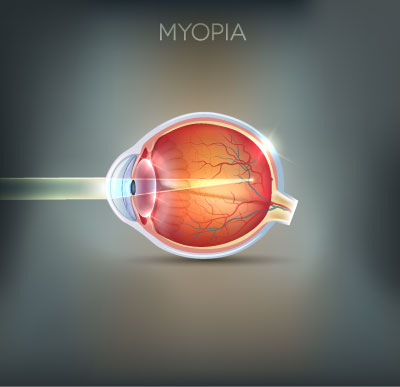
Myopia (Short-sighted)
Myopia, commonly called shortsightedness, is a condition in which light is focused in front of the retina, resulting in blurred vision. Shortsighted people can often see reasonably clearly at short distances, but will not be able to see distant objects clearly.
There is currently no cure for myopia, but spectacles, contact lenses and refractive surgery can all provide good distance vision for people with myopia.
The exact causes of myopia are not known. At various times people have blamed excessive amounts of reading, poor metabolism, poor diet, poor light, poor posture and genetic factors.
Recent research has shown that the development of myopia is influenced by both genetic and environmental factors.
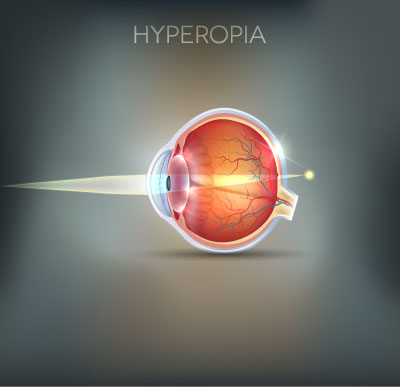
Hyperopia (Long-sighted)
Hyperopia or long-sightedness is a condition in which the optical components of the eye are not strong enough, and so light is not focused onto the retina. This results in blurred vision that is usually worse at shorter distances.
People with hyperopia often have reasonable vision in the distance, but may find that their vision is blurred or that they experience feelings of eyestrain or headaches when doing near work, such as reading or computer work.
It tends to increase, but not always. We all find it harder to focus on close objects as we get older. Hyperopes have trouble sooner and may need reading spectacles earlier because they have to focus more to start with.
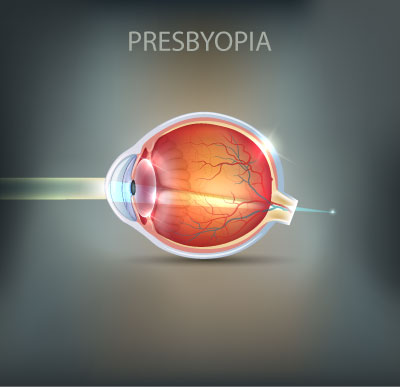
Presbyopia
Presbyopia is the gradual reduction in the amount that the eye can change its focus. The changes are the result of the continued growth of the biological lens inside the eye, and are a normal part of ageing.
Presbyopia usually becomes noticeable between the ages of 40 and 50 as an inability to focus on near objects. People in this age group often find that they have to hold things further away to see them clearly.
Presbyopia can be corrected by an optical prescription specifically designed for close work. This can be provided in many forms, including reading glasses, bifocals, trifocals and progressive lenses (multifocals).
COMMON EYE CONDITIONS
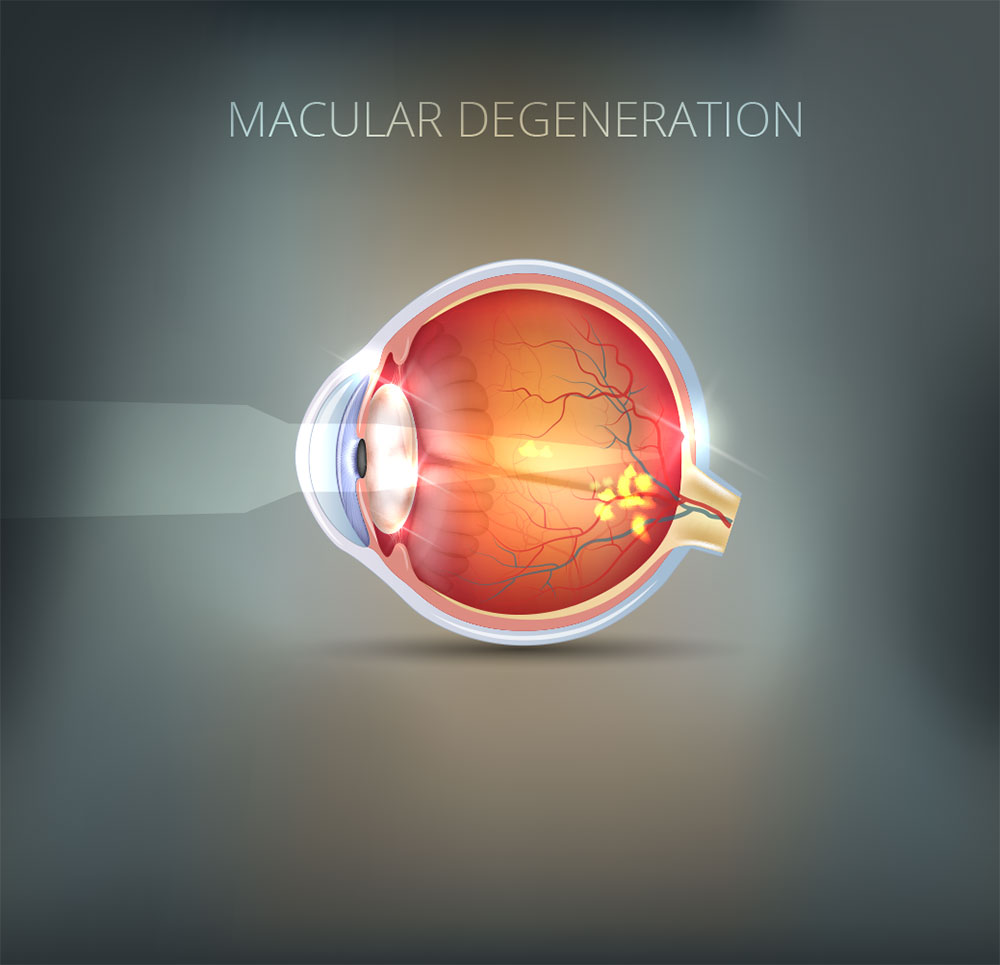
Age-related macular degeneration
This is a progressive condition that can affect people as they get older. It tends run in families. There are different forms which have different outcomes for vision. AMD accounts for 45% of people over 70 years of age who are registered as legally blind. With macular degeneration central vision does become severely affected but sufferers will retain a certain level of peripheral vision.
What causes AMD?
AMD is the result of ageing processes in the eye. The macula (responsible for central vision) suffers “wear and tear” over time and it is believed that a build up of waste material at and around the macula is the reason for the reduction in vision that occurs in this condition.
Symptoms: There are two types of AMD, Dry and Wet.
Dry AMD is the most common form of the condition and usually causes gradual changes in vision. Wet AMD affects a much smaller percentage of sufferers and is usually of sudden onset with significant and obvious reduction in vision. In Wet AMD, abnormal blood vessels develop beneath the macula and begin to leak.
How is AMD detected and diagnosed?
People with AMD may notice that their vision has deteriorated. Optometrists perform a number of tests in an examination that enable them to detect the presence of AMD in the early stages.
The optometrist examines the macula carefully with an instrument called an ophthalmoscope that allows examination of the interior of the eye. Sometimes the optometrist may place a drop in the eye to dilate the pupil to get a better view of the internal structures. Another test that may be used is a grid pattern known as an Amsler chart. Patients with AMD often report that sections of the grid appear to be distorted or missing. Optometrists will usually refer patients whom they suspect have AMD to an ophthalmologist (eye specialist) for confirmation of the diagnosis.
Treatment:
There is no way to reverse the damage done to the retina in AMD. Where new blood vessels have appeared in the macula area (Wet AMD), laser surgery or anti– VEGF therapy (injections into the eye) may be used.
These treatments are most successful in the early stages of the condition.
What should you do to avoid AMD?
Regular eye examinations are the key to early detection of retinal changes and other signs of disease. If you notice any change in the quality of your vision, have your eyes examined immediately. Regular examinations are particularly important for people over the age of 50 years and people whose families have a history of eye conditions.
The latest research advises that diet can be useful. smoking has been indicated as a risk factor for developing the condition. Some people are advised to take oral vitamin supplements to reduce the risk of developing AMD, always consult your optometrist or ophthalmologist before taking any such supplements.
The following fruit and vegetables have been reported to have some effect in reducing the risk of developing AMD
Yellow / Orange – corn, oranges, squash
Green – kale, broccoli, cabbage
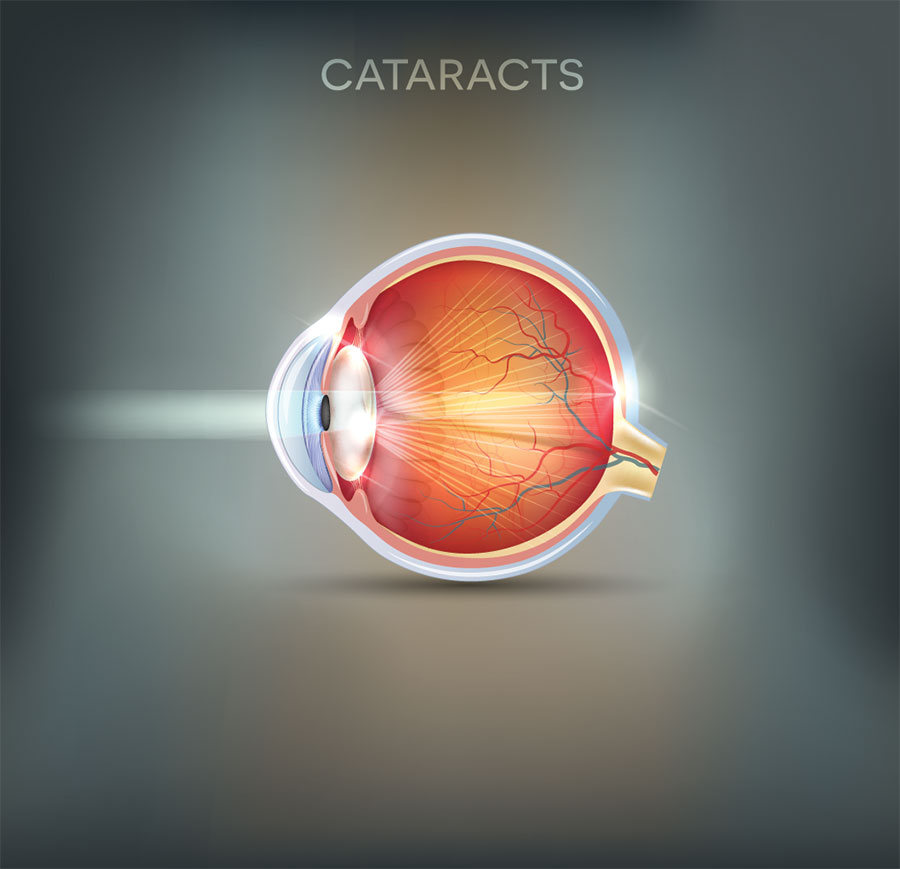
Cataracts
A cataract is a very common condition, affecting mostly older people. It is said “everyone will eventually develop a cataract if they live long enough”.
What is a cataract?
Basically there is a lens in the eye that controls focusing. As a person ages this lens can become cloudy which dims the vision, like looking out of a dirty window. There are many different types of cataract depending on which part of the lens is affected and the underlying cause. Not all types of cataract are the same and not all will develop in a similar manner. However, the majority of cataracts are seen in older people.
How will I know I have a cataract?
A person with an age related cataract might find that they can’t see as well as they used to or that their vision in general is “dimmer” than before. They may also suffer from glare. Their prescription may have changes suddenly after a long period of stability. The change is often gradual and is painless and in many cases a person may not have any symptoms in the early stages of cataract development.
How is a cataract treated?
Cataracts can be treated by means of a very simple procedure, which is usually carried out under local anaesthetic as an out patient procedure in a hospital. When to treat a cataract is a decision for the eye specialist (ophthalmologist) but your optometrist will advise you if / when you will need to consult an ophthalmologist. UV exposure has been linked to cataract development, so wearing well fitting sunglasses with full UV protection and good coverage can help reduce your risk of cataract development.
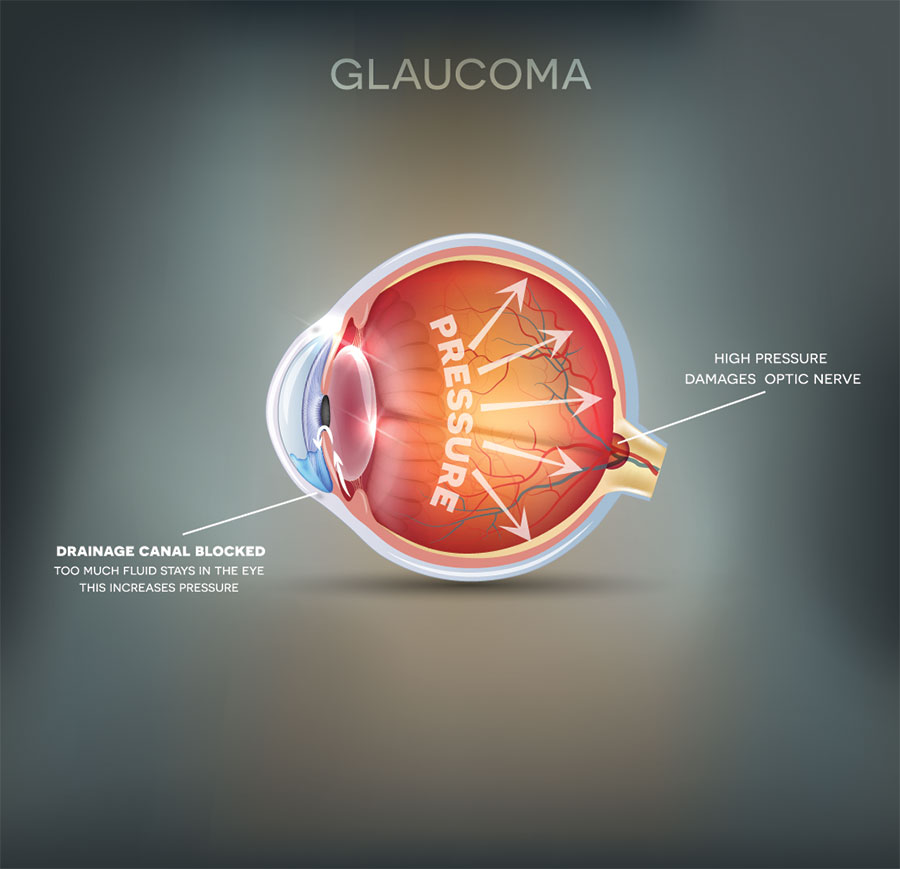
Glaucoma
Glaucoma is a condition in which the nerves which transmit information from the eye to the brain become damaged. It is often associated with a build-up of pressure in the eye. In some forms of glaucoma, the pressure inside the eye can become extremely high, but in other forms the pressure may remain normal. If untreated, glaucoma can cause blindness. Initially peripheral vision is affected but the damage extends if not treated. The damage to the nerve cells cannot be reversed although it is often possible to prevent further damage. The longer the disease is left untreated, the greater the likelihood of damage.
Who is at risk?
People over the age of 40 years are far more likely to have glaucoma than younger people. Also, glaucoma tends to run in families.
What causes glaucoma?
The exact causes of glaucoma are not known. In some cases the drainage network of the eye may not be formed properly, or may become blocked by natural materials or due to injury; in other cases there is no clear cause.
How can I tell if I have glaucoma?
It normally develops over a period of time without any pain or blurring of vision. Glaucoma affects peripheral or side vision first, allowing perfect central vision to be maintained for a long time, when this remains normal we may not notice other changes in peripheral vision.
How can the condition be detected?
The optometrist looks at the nerve fibres at the back of the eye, measures the pressure in the eye, and tests the field of vision. These tests are simple and painless. It was once believed that the eye pressure was the single cause of the condition, we now know that people with normal eye pressure may also develop the condition.
Treatment?
Eye drops are usually used to treat glaucoma. Surgery may be necessary if there is a blockage in the drainage system and the pressure cannot be reduced.
Acute Angle-Closure Glaucoma :
There is a type of glaucoma called Acute Angle-Closure Glaucoma. This has a sudden onset. It can cause the affected eye to be very sore and red, and can produce other symptoms such as noticing haloes around lights, vision loss and headaches. The symptoms may occur in episodes with each episode lasting for a number of hours and causing permanent damage to vision. This type of glaucoma requires emergency treatment by an ophthalmologist.
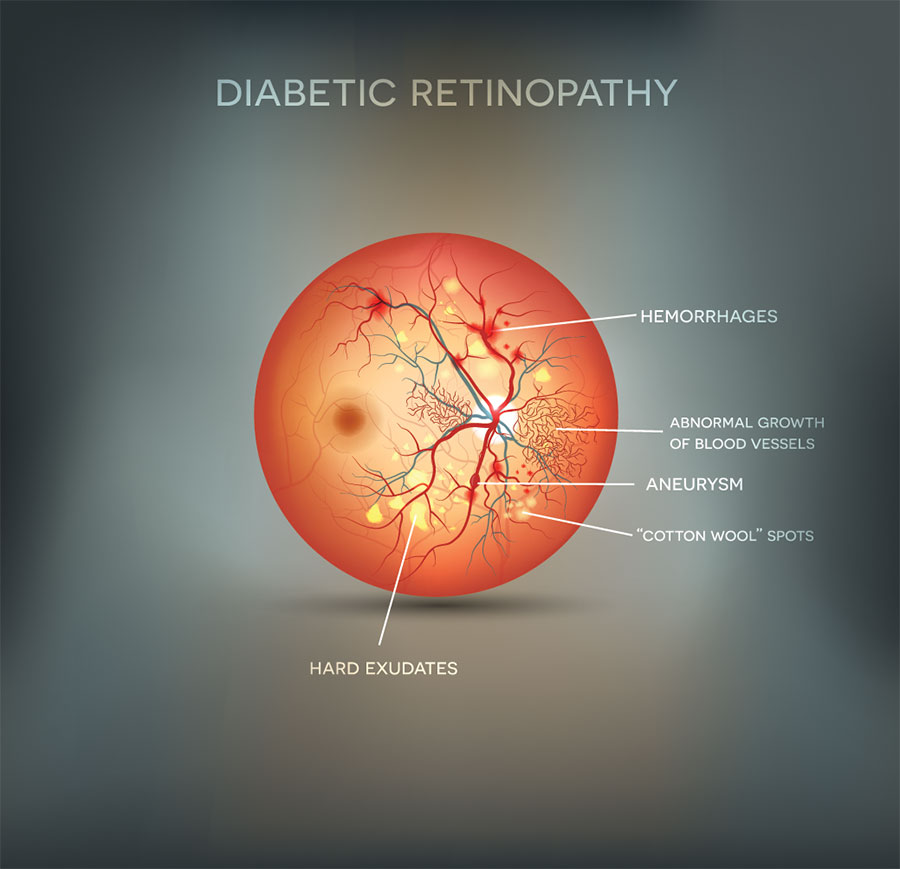
Diabetes and the Eye
Diabetes related eye disease is the leading cause of vision loss in adults of working age (20-65) in industrialised countries. 5.4% of females and 4% of males in the Repubic of Ireland have been diagnosed as having diabetes. 74% of those who have diabetes for over 10 years will develop diabetic eye disease.
Types of Diabetes:
There are two main types of Diabetes, early onset (Type I) and late onset (Type II). Both forms of Diabetes can cause damage inside the eye. Early intervention is essential to avoid visual loss. Diabetes sometimes causes vision to fluctuate from day to day or throughout the day. This symptom can often be the first indicator for an optometrist that a patient could have diabetes. If diabetes is diagnosed, good blood sugar control should stabilise vision. Over time, particularly in poorly controlled diabetes, serious retinal damage can occur.
Diabetic retinopathy:
After diabetes has been present for some years, changes may occur at the back of the eye in the retina. These changes are known as diabetic retinopathy. The risk of developing retinopathy increases with the length of time you have had diabetes. The risk is also increased when there is poor control of blood sugar levels. As diabetic retinopathy develops, blood vessels at the back of the eye leak and if left untreated a person could lose their sight altogether. Whilst not all those with Diabetes will develop Diabetic Eye Disease, it is essential to have regular eye tests to examine behind your eye even if you feel your eyesight is “fine and clear”.
Often your optometrist or ophthalmologist will put some drops in your eyes to “dilate” them, which makes the pupil larger and allows a more detailed examination of the back of your eye. The best way to attempt to avoid developing diabetic eye disease is to maintain blood sugar levels at advised by your doctor and attend for regular check ups. It is also recommended that you see your optometrist at least annually for a dilated eye examination.
Treatment:
Diabetic retinopathy will often be treated with a laser, which helps to stop leakage from the blood vessels at the back of the eye. Regular eye examinations and good control of blood sugar levels should help reduce the likelihood of this treatment being necessary.
